An outbreak of Ebola for nurses positioned on the front lines will likely tap them as the first responders to correctly assess cases. For more than thirty years Ebola has been feared as a potentially cataclysmic epidemic. “The Hot Zone” and other sensational books and movies have promoted this fear.
Today we finally have an Ebola epidemic and it has now reached crisis proportions in West Africa. So, this article explains Ebola from the nurse’s perspective. Positioned on the front lines of medicine, nurses will likely be the first to correctly assess Ebola cases.
What is the Ebola Virus?
Featured Programs
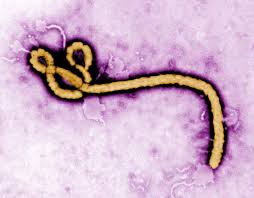
Ebola belongs to the obscure Filoviridae Family and includes both the Marburg and Ebola filoviruses. The Ebola virus is simple in design and only has only about a dozen genes. It has a filamentous form and can also appear in various shapes that include “U”, “6”, as well as branched filaments. Furthermore, individual virus filaments can measure up to 14 micrometers in length.
In humans, the virus causes Ebola Virus Disease (EVD) also known as Ebola Hemorrhagic Fever (EHF). Five species of Ebola are known so far: Tai Forest (TAFV), Zaire (EBOV), Sudan (SUDV), Bundibugyo (BDBV), and one of apparently Asian origin – Ebola Reston (RESTV). Filoviridae virus particles are environmentally stable. Research indicates that both Ebola and Marburg are stable in small particle aerosols. Aerial transmission is a possibility.
Ebola and the Immune System
Suppression of the immunological system is severe. Therefore, damage to the spleen and lymph nodes is notable. Fatal cases have necrotic lesions and extensive bleeding from tissues and organs throughout the body. The virus also attacks the vascular system. Both kidney and liver failure are likely outcomes.
Once patients are symptomatic viral particles are found throughout the body including the skin. Recovering survivors generate significant levels of antibodies for Ebola and are immune to further infection. This immunity is believed to last at least ten years.

Ebola Occurrence
Understanding the geography of Ebola is important. The current outbreak likely began in Guinea and has spread to neighboring Sierra Leone, Liberia, Senegal, and even to more distant Nigeria and also Mali. Past known Ebola outbreaks have occurred throughout West Africa including Zaire, Sudan (1979), the Republic of the Congo (1977), Uganda, South Africa, and Reston Virginia (1992 and again in 1996).
The Reston outbreaks were vectored by infected research monkeys shipped into the U.S. from the Philippines. The South African outbreak was also “imported” by a traveler who may have actually been exposed in Zimbabwe.
The geography of Ebola is also represented by the following alphabetical list of countries where the infection has occurred. Highlighted countries are in the current 2014 West African outbreak.
- Congo (Republic of Congo)
- Gabon
- Guinea
- Ivory Coast (Cote d’Ivorie)
- Liberia
- Mali
- Nigeria
- Senegal
- Sierra Leone
- Sudan
- Uganda
- Zaire
How Ebola Spreads
What this distribution clearly illustrates is that modern societies are interconnected by many modes of travel, and contagious persons can quickly cross nations and international borders. This means that new cases and clusters can appear in unexpected places. This happened in Dallas, Texas (2014).
The Discovery of Ebola antibodies in local populations now indicates that the disease is more common than previously appreciated. In Gabon, 15% of the local population has tested positive for Ebola antibodies. This may indicate that some people are exposed to the virus without suffering serious illness.
The first western outbreak of a filovirus occurred in 1967, in Marburg Germany. A total of 31 human cases resulted from contact with African green monkeys used for research. The resulting human mortality rate from the Marburg Virus was 23%. Reported virulence of Ebola in Africa has ranged from 100% to 50%.
Filovarae is zoonotic and known vectors include humans, monkeys, apes, other primates, Fruit and Rousettus bats, and pigs (recently detected in Southeast Asia). Medical personnel who treat Ebola patients or work in emergency rooms, ambulances and first-response personnel, and their family members are also highly susceptible.
Inorganic vectors include physical contact with contaminated hospital equipment, bedding, cleaning materials, patient care products, needles, and other sharp objects, as well as objects handled and surfaces contacted by the infected patient or contaminated by the patient’s bodily fluids.
Symptoms
Patients become symptomatic within 2 to 21 days of exposure and commonly within 8-10 days. Patients will present with fever (>38.3C / >100.9F).
The disease initially presents with flu-like symptoms. These include malaise, confusion, fever, headaches, abdominal pain, miscarriages, watery eyes, diarrhea, and even hiccups. At this point, Ebola is infectious for another 14-21 days. Afterward, the body continues to shed viral particles but this recovery phase is not infectious. However, seminal fluid can remain infectious for 3 months after recovery (no sex for three months).
Advanced Symptoms
As the infection advances effects can include cytosis, the prevalence of cytokines in the blood, necrosis of organs, rupturing of endothelial cells lining the body’s vascular network, severe kidney and liver damage, and damage to the eyes caused by ruptured capillaries. Bruising, bleeding from bodily orifices, bloody stools, and bloody diarrhea are symptomatic of late-stage infection.
The human immunological system is overwhelmed. Severe headaches, severe abdominal pain, diarrhea, swollen lymph nodes, bodily rashes, watery eyes, and mucosal discharges from bodily orifices are symptomatic.
Death occurs from septic shock, loss of blood, vascular and cardiac complications, kidney and liver failure, and complications from severe dehydration.
Recommended Diagnostics
Recommended lab diagnostics include the antigen-capture Enzyme-Linked ImmunoSorbent Assay (ELISA) and IgM ELISA; Polymerase Chain Reaction (PCR); and, microscopy to visually identify the virus. Testing should be limited because the presence of any patient samples increases the risk of virus transmission and infection.
However, healthcare workers should test symptomatic patients daily. Patients in the early stages of infection have sometimes tested false-negative. Again, daily testing on symptomatic patients is required..
False Alarms
Malarial infections present in a similar manner during the early infectious stage. Additionally, other tropical diseases including Chikungunya, Yellow Fever, Typhoid, Cholera, and Dengue may have symptoms similar to early-stage Ebola infections.
Diagnosis should include a clear understanding of the patient’s recent travel history in known Ebola regions (see occurrence section above) and possible contact with known Ebola vectors. Other indications may include any bloody bodily fluid discharges or bloody stools.
Isolation
Symptomatic patients are highly contagious. Therefore, effective isolation is absolutely required. Nursing must be delivered through isolation barriers by staff wearing full-body personal protection equipment (PPE). No portion of the body can be exposed. Mucosal-lined passages of the mouth and nose should be properly protected by appropriate masking in accordance with the hospital’s protection management standards for highly infectious diseases.
Isolation wards must be routinely disinfected and protective materials replaced. The resulting waste is a biological hazard and should be disposed of by high-temperature incineration into ash, or by carefully following hospital-approved autoclave procedures for highly infectious diseases.
Personal Protection
Contact with their bodily fluids can transmit Ebola. Bodily fluids include blood, plasma, perspiration, saliva, sputum, breast milk, tears, feces, seminal fluid, and vaginal discharges. Coughing and even talking could present infection risks from sputum aerosols.
Especially vulnerable entry points would include the eyes and surrounding tissue, mouth and nostrils, and exposed cuts or abrasions on the skin. This requires full-body covering, including full-face protective masks. All personal protection equipment (PPE) should be disposable and discarded after a single use. Also, the reuse of PPE increases the possibility of accidental infection.
Ebola Treatment
Dr. Adaora Igonoh is a physician practicing in Nigeria who recommends aggressive rehydration. As an Ebola survivor, Dr. Igonoh drank daily at least 5 liters (1.3 gallons) of water fortified with saline and glucose. Her illness had already progressed to mouth sores, sore throat, vomiting, and malaise when she began aggressively rehydrating. Maintaining electrolyte balance is also important.
Oxygen should be administered throughout the treatment phase. Also, avoid anti-inflammatory drugs because they suppress an already over-taxed immune system. Avoid Aerosol Generating Procedures (AGP) and also any contact with aerosols as sputum aerosols may transmit the virus.
The US CDC (Centers for Disease Control) recommends only using EPA registered hospital-grade disinfectants specifically approved for non-enveloped viruses. These would specifically include disinfectants approved for adenovirus, norovirus, polio, and rotavirus.
Field Disinfection
For field disinfection, CDC recommends strong solutions of 0.5% (5000 ppm) hypochlorite (bleach), and a skin-safe 0.05% (500 ppm) solution for hand washing and cleaning of chlorine-sensitive tools and equipment. Nurses should also use hospital-grade alcohol-based disinfectants.
A number of new anti-viral medicines are appearing and the status of these changes frequently. So, nurses should seek guidance to best understand the current outcomes for these experimental drugs.
Surveillance
Survivors generate antibodies for at least 10 years and during this time are not likely to become reinfected. However, we do not know if this immunity lasts for life. Additionally, we do not know if acquired immunity for one filovirus species extends to others. So, reinfection can happen with a different filovirus species.
Long-term complications from the disease include joint pain, vision complications, vascular, kidney, and also liver problems. Survivors should abstain from sex and any form of intimate contact that includes the exchange of bodily fluids for at least 3 months after clinical discharge.
Helpful Resources
CDC: http://www.cdc.gov/
CDC Guidance Help Line: 1-800-CDC-INFO (1-800-232-4636)
EPA-registered disinfectant lists: http://www.epa.gov/oppad001/chemregindex.htm/
Ebola Triage Checklist
- Detain and Isolate the symptomatic patient.
- Don appropriate full-body PPE. Use disposable PPE and discard it after a single use.
- Notify Hospital Staff and Management
- Ensure that the County Health Department is also notified
- Notify the State Health Department and CDC
- Isolate Patient in a Contained Environment suitable for highly infectious diseases.
- The room should include an attached/dedicated bathroom.
- The isolation room should also have a door, air micro-filtration, and a pressure differential that prevents air from leaking out of the room and into adjacent hospital workspaces.
- Clearly mark the outside of the door as RESTRICTED ACCESS.
- Post a guard to control access to the patient, using the access list.
- Limit staff and restrict visitors to minimize exposure.
- Maintain an access list.
- Identify and list all persons who have had recent physical contact with the patient.
- Immediately remove all soiled bedding and other material
- Clearly label and carefully handle waste as a bio-hazard
- Avoid Aerosol Generating Procedures (AGP)
- Administer aggressive rehydration and monitor electrolytes
- Administer oxygen
- Treat secondary infections
- Minimize lab testing to reduce transmission risk
- Perform ELISA and PCR testing to confirm filovirus. Retest at least daily to ensure negative tests are not false-negative.
- Avoid anti-inflammatory drugs as these may suppress the patient’s immune system
Related: